-
-
Access Free Student Software
Ansys empowers the next generation of engineers
Students get free access to world-class simulation software.
-
Connect with Ansys Now!
Design your future
Connect with Ansys to explore how simulation can power your next breakthrough.
Countries & Regions
Free Trials
Products & Services
Learn
About
Back
Products & Services
Back
Learn
Ansys empowers the next generation of engineers
Students get free access to world-class simulation software.
Back
About
Design your future
Connect with Ansys to explore how simulation can power your next breakthrough.
Free Trials
ANSYS BLOG
September 25, 2019
What is PMMA and How Is It Used in the Medical World?
Poly(methyl methacrylate), or PMMA, is known by many different names, including Plexiglas and acrylic. The biocompatibility of PMMA material has gained it the medical moniker of “bone cement.”
PMMA is often used as a lighter, shatter-resistant alternative to glass in everything from windows, aquariums and hockey rinks. Therefore, it’s hard to fathom that this easy-to-process, low-cost, versatile material is also used in dentures, bone implants and more.
Despite being formed by polymerizing methyl methacrylate (MMA) — an irritant and possible carcinogen — PMMA is extremely biocompatible.
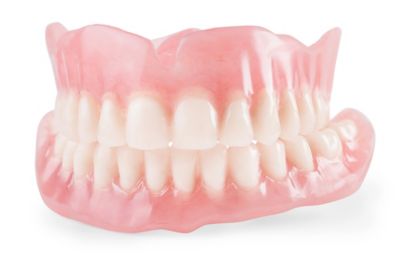
The biocompatibility of PMMA material makes it great for
denture manufacturers.
This biocompatibility can be attributed to PMMA’s resistance to:
- Temperatures stress
- Chemical reactions
- Human tissue
- Bioprocesses
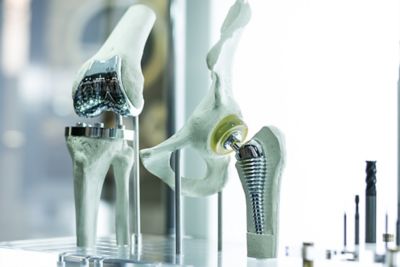
As bone cement, PMMA is used to fill in the gaps between implants and bones. PMMA material is good for this procedure because it is biocompatible and simple to polymerize within a hospital environment.
However, a better understanding of material intelligence can help answer whether PMMA is always a good option for in vivo implants.
Though PMMA Material Is Biocompatible, Is It Always the Best Medical Option?
In an operation room, bone cement is made from a powder and a liquid. The powder is composed of MMA copolymers while the liquid contains MMA monomers and chemical accelerators and inhibitors.
Mixing the powder and liquid creates a putty which can be applied between the bone and the implant. Think of the putty like the grout between tiles: It anchors the implant to the bone.
However, there are a number of reasons why PMMA material is not ideal for this job:
The biocompatibility of PMMA material makes it a go-to option to anchor implants to bone. But is it the best option?
- PMMA’s fracture toughness is between 0.7 MPa∙m1/2 and 1.6 MPa∙m1/2, while bone’s fracture toughness is between 3.5 MPa∙m1/2 to 6.6 MPa∙m1/2.
- PMMA has a high polymerization temperature.
The difference between the fracture toughness of PMMA and bone can lead to impacts breaking the cement in scenarios where the bone or implant is unaffected.
Also, research has shown that, due to exothermic polymerization, the putty can reach temperatures above 80 C outside the body and around 50 C inside the body, damaging the bone. This translates to a longer recovery time for patients.
Furthermore, small amounts of unpolymerized MMA can remain in the cement. These components can find their way into the rest of the body causing hypotension.
PMMA may have its issues as bone cement, but it’s still the best material option in many situations. However, researchers are looking for a better material for bone cement purposes.
Doctors Benefit from the Biocompatibility of PMMA Material
PMMA is an important material for many other medical procedures. For instance, it is used to make dentures and fillings because it is easy to dye and quick to form.
As a result, doctors can use PMMA material to make dentures and fillings that closely match the size and color of the original teeth.
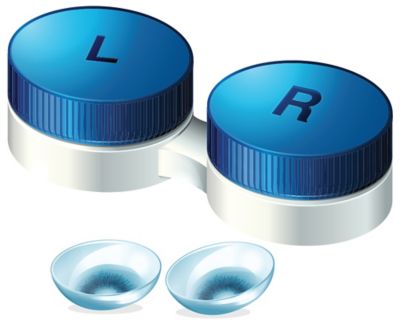
PMMA material has also made it into the eye. Historically, it was used as hard contacts or intraocular lenses.
The ocular use of PMMA started through a surprising discovery. An ophthalmologist working with the Royal Air Force, Sir Harold Ridley, noticed that splinters of PMMA in the eye — resulting from shattering windshields — did not trigger the same rejection as glass splinters.
The biocompatibility of PMMA material made it a great choice for hard contacts and intraocular lenses. However, softer materials have dominated the market.
This led Ridley to try using PMMA to replace damaged lenses in people suffering from cataracts. He achieved permanent implantation in 1949 at St. Thomas Hospital.
A number of PMMA-based copolymers and silicone-based materials now compete with PMMA in the intraocular lens market. These materials have the advantage of being flexible and therefore less brittle.
In the case of contact lenses, soft lenses can be more comfortable. Additionally, with recent advancements in oxygen transmissibility, soft contacts tend to be the preferred option for patients.
PMMA material has many uses in the medical industry. Although it has become less common, advances in PMMA and similar materials will continue to improve the lives of many.
To learn more about how material intelligence can improve people’s lives, access medical materials information sources here.
This blog takes notes from Sean Newham's blog that was previously on the Granta website.